Our allergy guide is designed to assist you in safely introducing allergenic foods to your baby, minimising the likelihood of food allergies developing and helping you understand what to do in case a reaction occurs.
Food allergies are no joke! Their PR team have done wonders in the past decade spreading the word that they’re not to be taken lightly. However, unless you have personally experienced an allergic reaction or witnessed it happening to someone close to you, it may be challenging to fully grasp the seriousness of this situation.
In recent years, the prevalence of food allergies among children has reached alarming levels, affecting approximately 1 in 10 kids in Australia. As parents, we often experience anxiety when introducing allergenic foods to our babies, but delaying their introduction can actually increase the risk of developing food allergies.

- When should I introduce allergens to my baby?
- How do I introduce allergens to my baby?
- Top points to consider when introducing allergens are:
- Signs of an allergic reaction:
- What to do if my baby has an allergic reaction?
- How do you diagnose a food allergy?
- Top 10 ways to manage a food allergy in babies and children:
- Top food swaps for cooking with allergies:
- Helpful Resources:
When should I introduce allergens to my baby?
The ASCIA (Australian Society of Clinical Immunology and Allergy) Recommend introducing all common allergens before 12 months of age to reduce the likelihood of allergies developing. You should start introducing allergenic foods when your baby starts solids around 6 months.
These common allergens are:
- Peanut
- Tree nuts (such as: almond, brazil nut, cashew, hazelnut, macadamia, pecan, pistachio and walnut)
- Egg
- Fish
- Shellfish
- Dairy
- Wheat
- Soy
- Sesame
How do I introduce allergens to my baby?
I like to conservatively start their digestive systems on gentle veg/fruit purees, then meat purees and then after 2 weeks begin introducing the allergens, but this is not a hard and fast rule! Feel welcome to introduce them sooner if you’d like.
For allergens that are more likely to cause anaphylaxis (like peanut, tree nuts, seafood, milk, wheat and egg) start by:
- Rubbing a tiny amount of the allergen (like a smooth nut butter) inside your baby’s lip. If no reaction, then increase that amount the next day or two. If still no reaction then you can begin mixing that ingredient into your baby’s puree or including it with their finger foods if BLW like a bit of nut butter spread on a toast finger or a piece of banana.
- Mixing ¼ teaspoon of the allergen such as fully cooked egg yolk, nut butter or blended fish into their puree. If no reaction, increase to ½ teaspoon the following day or two. If no reactions occur you should continue to include this allergen in your baby’s diet 1-3 times a week.
Top points to consider when introducing allergens are:
- Only introduce one allergen per meal per day so that it can be identified if there is an allergic reaction.
- If your baby does have an allergic reaction, stop giving that food immediately and seek medical advice.
- When offering food to your baby, always choose the right textures that align with their developmental stage. Use nut spreads or flours to prevent choking. Do not feed your baby whole nuts or nut pieces.
- Wait 3-5 days between introducing different allergenic foods to confidently identify a reaction.
- Once a food has been introduced safely to your baby with no allergic reactions, continue to include that food in your baby’s meals as part of a varied diet.
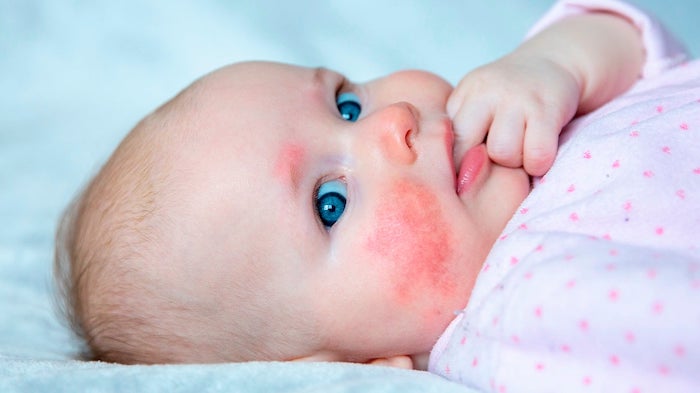
Signs of an allergic reaction:
Reactions occur quickly, usually within a few minutes and can be really mild to really scary (severe). Your baby may display one or more of the following signs:
- Sudden irritability
- Grabbing at ears / mouth / nose / throat
- A pink or red rash around the mouth or face with or without hives
- Red, itchy, watery eyes
- Sneezing
- Blocked nose
- Wheezing or coughing
- Less sudden allergic reactions can result in digestive upsets over the next few days which is why it’s important to split the introduction of different allergenic foods apart by 3 to 5 days.
- For more detailed information and signs of anaphylaxis, refer to this helpful webpage https://preventallergies.org.au/identifying-allergic-reactions/
IMPORTANT NOTE Your baby may not react the first time you’re introducing them to that food. Sometimes, the first exposure is the immune system’s priming dose and the second time you give them that food will be the one that will cause the reaction. If this is the case, the more and more times your baby is exposed to that allergen, the worse the reaction will get which can eventually lead to anaphylaxis.
What to do if my baby has an allergic reaction?
- If your baby reacts to a food, you must immediately stop giving them that food and remove it.
- Consult your GP who may refer your baby or child to an allergy specialist or immunologist.
- An antihistamine may help calm the symptoms but this is not advised unless directed by your childs doctor for infants under 2 years.
How do you diagnose a food allergy?
Allergy Testing
If your baby hasn’t tried many allergens yet but has reacted to one, your specialist can provide further testing such as:
- A painless skin prick test to confirm the suspected allergy and identify whether your baby or child may have allergic responses to other allergenic foods.
- IgE blood test – an allergy test that checks for antibodies called immunoglobulin (IgE) in your blood. An example where this can be helpful is when finding out the severity of a peanut allergy as the test determines the amount of antibody to total peanut and the amount of antibody to specific peanut components. This may help in finding out if the allergy may become anaphylactic.

Top 10 ways to manage a food allergy in babies and children:
- Know their symptoms.
- Get a professional medical diagnosis.
- Create an emergency action plan with your child’s specialist like this one: https://www.allergy.org.au/images/stories/anaphylaxis/2023/ASCIA_Action_Plan_Anaphylaxis_Red_General_2023.pdf
- Learn how to use an auto-injector (epi-pen).
- Always read food labels.
- Avoid the chance of cross contamination when eating at home, in restaurants or at someone’s house.
- Teach your child to always ask if the allergy is present in food offered to them by others.
- Ensure your child’s daycare or school are aware of their allergy and have their action plan and medication in case a reaction occurs.
- Pack a lunch for your child if you aren’t certain there will be safe food options for them when out of the home. Hot tip: Bring an allergy free cupcake for them to enjoy when attending birthday parties.
- Ensure your child knows how serious their allergy is to prevent life-threatening exposures and how to call for help in case one occurs.
Top food swaps for cooking with allergies:
Nuts: Sunflower seed butter, plain greek yoghurt, regular butter, Nuttelex butter
Sesame/ Tahini: Sunflower seeds/ sunflower seed butter, poppy seeds, chia seeds
Egg: Apple sauce, banana, chia egg (1tbsp chia seeds + 2.5tbsp water = 1 chia egg)
Dairy Milk: Any dairy alternative will work such as almond milk, hemp milk, cashew milk, oat milk, soy milk.
Wheat/ Gluten: Always check specific recipes as different flours need different ratios of wet/dry ingredients but popular substitutions to wheat flour are chickpea flour, tapioca flour, almond flour, buckwheat flour, amaranth flour, quinoa flour and arrowroot flour
Soy: Tamari, coconut aminos, liquid aminos, fish sauce, worcestershire sauce.
As a parent of a child who is anaphylactic to peanuts, the mere thought of his exposure to this life-threatening allergen in a school environment is truly terrifying. Parents may sometimes feel frustrated by the “No Nuts” policies in schools or early childhood settings. It’s crucial, however, to remember that as inconvenient as it may seem to avoid packing certain foods that your child enjoys, we must respect the potential life-threatening risks they pose to other children. For instance, a seemingly harmless peanut butter sandwich or hummus dip could trigger a severe allergic reaction in another child.
Helpful Resources:
- https://www.allergy.org.au
- https://allergyfacts.org.au
- https://preventallergies.org.au
- https://www.rch.org.au/allergy/
Disclaimer: The information provided in this blog article is intended for general advice and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your healthcare professional or qualified medical practitioner with any questions you may have regarding a medical condition.






